 By Liam Neyland How often have you heard the phrase ‘Put some ice on it’? Whether you’re young or old, someone at some point would have recommended this, maybe even a health professional like your local GP. The reason this saying is used so frequently is due to the RICER method. For those of you who are unfamiliar with this, RICER is an acronym used in the health profession to treat acute injuries. It stands for rest, ice, compress, elevate and refer, and is a step-by-step guide on how to approach at home care of acute pain caused by an injury. This form of treatment was originally coined in 1978 by Dr Gabe Mirkin, an American sports doctor. However, latest research indicates that the use of ice may have a more negative impact on the healing of acute injuries than initially thought.  Just like technology the medical industry is constantly in a state of fluctuation and adaption to find the best guidelines for treatment. This can be both a blessing and a curse as age old advice that has been around for 30+ years has become a household go to, may now be no better than doing nothing, so the question is why the sudden change? Recent research has found that post soft tissue injuries initiate an inflammatory phase in which special inflammatory cells recognise damage has occurred to the extracellular matrix (large network of molecules that surround, support and give structure to tissue and cells). When this happens immune cells such as neutrophils and macrophages are recruited to clear up damage and perform phagocytosis (eating excessive debris). Further, processes occur such as the secretion of growth factors as well as a myriad of other functions which are designed to move, rebuild and produce cells as well as blood supplies. This whole process is pro-inflammatory which means it happens the moment the affected limb or area starts to swell. The reason this is important is that the use of ice could negatively affect this process. Ice is a vasoconstrictor, which means it limits blood supply to the area thus reducing swelling. By reducing the blood supply and swelling, it takes longer for important cells to reach the area and delays the process of healing. Knowing all that, you may be asking what should we do for acute injury management? This is where the new acronym PEACE and LOVE come into place. PEACE and LOVE is the most up to date method recommended in treating acute soft tissue injuries. For the first few days of an injury PEACE is used. P- Protect: De-load the affected limb or area for the first couple of days. This does not mean avoidance of movement but instead gentle pain free motion with little to no loading. E- Elevate: Like the original RICER method, elevate the affected limb to the best of your ability, higher than hips for lower limb and higher than the heart for upper limb at a bare minimum. A- Avoid...items that may negatively impact the inflammation process such as ice or anti-inflammatory medication. C- Compress: Use compression garments and taping to limit tissue haemorrhage and joint oedema. E- Educate: Understanding what is happening in the body and it’s tissues is an invaluable tool in recovery to know the next best step as well as have realistic expectations of recovery time frames. After the initial 1-3 days of using plenty of PEACE is when we start to introduce some LOVE to the affected area or limb. L- Load: Use of early mechanical stress with loading promotes repair and builds soft tissue tolerance, be mindful to perform when little to no pain is present. O- Optimism: The brain is a power aspect in injury and recovery as studies have shown that having a brighter outlook can positively affect the recovery time frame. V- Vascularisation: Use of pain-free exercise that increases the resting heart rate can increase blood flow to injured structures positively affecting how the structure is handling load and how fast it can heal. E- Exercise: Specific rehab exercise program introduction With all that in mind it is important to understand that not all treatment is a one size fits all as every person is different. It can be difficult to understand and gauge the best approach to acute injuries, as for some individuals ice may be more beneficial due to the analgesic effects (pain relief) it provides. Being up to date on latest research as well seeking advice from qualified medical practitioners on best practice for you and your issue is important. References: Soft-tissue injuries simply need PEACE and LOVE - PubMed (nih.gov) Peace and Love Principle - Physiopedia (physio-pedia.com)
1 Comment
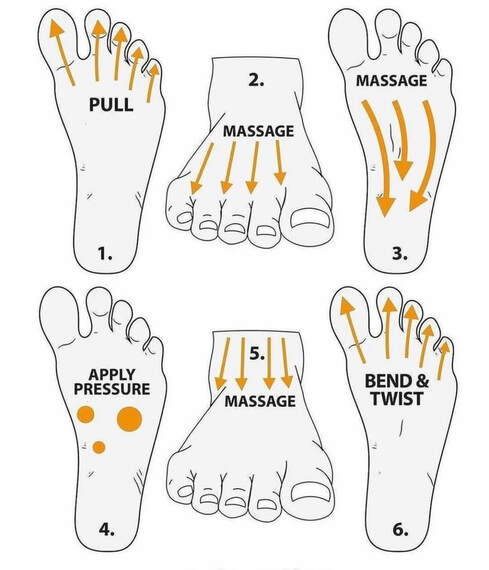
By Liam Neyland Recently I have had many patients ask me whether they should be taking magnesium supplements or increase their dietary intake. Magnesium is a crucial nutrient for the body’s health but has recently been labelled as a one size fits all cure. Today I am going to explain what the relationship between the body and magnesium, as well as the many benefits you may receive when increasing your daily intake. The relationship between magnesium and your body Magnesium in simple terms is one of the major minerals that the body relies on to function. As a matter of fact, every single cell in your body at any one time has some form of magnesium present, which it needs to properly function. One of the main roles that magnesium provides is to act as a cofactor (helper molecule) where it is involved in more then 600 reactions in the body. The main reactions magnesium plays a role in are energy production, protein formation, gene maintenance, muscle contractions and the regulation of the nervous system. Possible Benefits of High Magnesium Intake Boost Exercise Performance Magnesium is a major mineral used in the contraction of muscles all throughout the body. One of the major functions that magnesium has during muscle contraction is helping move blood sugar into the muscle, fuelling our overall muscle stamina. Magnesium also helps dispose of lactate which builds up during exercise and is the main cause of muscle fatigue. Help with depression Just like other parts of the body, magnesium plays critical roles in how our brain functions and it’s overall health. One of the more important roles magnesium conducts is the maintenance of NMDA receptors, which act as transmitters from the brain to the body and are needed for brain development, learning and memory. Certain studies have shown that an increased magnesium uptake can increase brain function, mood and even decrease risk of depression. Promote positive heart health Many things can play a role in overall heart health ranging from increased exercise, healthier diet and decreased alcohol intake, to name a few. However, increasing natural magnesium levels is underrated in the medical industry. Studies have shown links between high magnesium intake to lowered heart disease, stroke and high blood pressure. Other noteworthy benefits: • Helps fight inflammation by reducing CRP and interleukin-6 markers • Studies have shown a decrease in migraine severity • Premenstrual syndrome (PMS) symptoms can be relieved with magnesium intake • Increased bone strength and decreased risk of osteoporosis • Improved sleep quality and treatment of symptoms of certain sleep issues. • Helps alleviate symptoms of anxiety and stress  How can I improve my magnesium intake? One of the easier and most effective ways to increase our magnesium intake is to simply eat more foods that contain high levels of magnesium. The following foods are all rich in magnesium with some being higher in value depending on how you cook them. Foods like pumpkin seeds, chia seeds, spinach, almonds, cashews, edamame, peanut butter, black beans, salmon and brown rice are some of the heavyweights when it comes to magnesium intake. If for any reason introducing these foods may not be possible then you can simply balance out your intake through the use of supplements.  What are some negative effects of Magnesium? Magnesium on it’s own has little to no side effects when taken within it’s recommended daily intake. It has been recorded that an increase in magnesium through supplementation can cause nausea, vomiting and diarrhoea but these side effects are very rare. As long as the recommended 350mg daily limit is followed the likelihood of side effects are rare. It should be mentioned that unfortunately increasing your magnesium intake through supplementation is not viable for everyone, as some medications can have negative interactions. It is always recommended to discuss with your doctor if magnesium supplementation would be a healthy and safe option. How can my osteopath help? If you feel magnesium may be helpful in treating whatever ailment you could be suffering from but would like a second opinion, the Osteopaths at HMC are more than happy to answer any questions that you may have. References Magnesium in Human Health and Disease - Google Books Magnesium in Hypertension, Cardiovascular Disease, Metabolic Syndrome, and Other Conditions: A Review - Champagne - 2008 - Nutrition in Clinical Practice - Wiley Online Library Side Effects Of Too Much Magnesium - TheFitnessManual Most Common Magnesium Side Effects for Health - Kobmel 12 Magnesium Health Benefits (healthline.com)  By Angus Nicol After reading the first two blog posts you’re probably ready to throw your shoes out right now! But hold up there, partner. Our feet have become very accustomed to wearing shoes, so transitioning to barefoot walking can take some time and patience. It’s important that when you start walking barefoot that you start off slowly, even for as little as 15-20 minutes a day, and slowly increase the length of time. This will allow the muscles, tendons and ligaments in your foot to adapt without causing excessive load, stress or damage. You may wish to begin your barefoot journey inside on familiar surfaces, especially if you have balance issues. However, be aware that hard surfaces (eg concrete floors and tiles) will put more force and stress through your feet, so wooden or carpeted surfaces are preferable. You can also test yourself on outdoor surfaces, again seeking out relatively flat and semi- firm surfaces (eg turf/even grass, sandy beaches and/or rubber sports courts) but avoiding concrete/bichuman. You may also like to consider starting activities/exercise that require you to be barefoot - such as yoga, pilates or martial arts. If you are barefoot walking, please check your feet regularly for injury. Many people have conditions that lead to decreased sensation in the feet (a few examples include diabetes, peripheral neuropathies or circulation problems), therefore there is a risk of sustaining wounds without noticing and increasing risk of infection. I wouldn’t be a good osteopath if I didn’t at some point mention everyone’s favourite thing… REHAB EXERCISES (aka homework). When beginning your barefoot journey, you can help your foot to adapt more quickly by doing additional exercises to help relieve the muscles and joints in the foot to help them tolerate the changes better. The photo below shows some simple exercises you can do. These exercises can be helpful for people who have foot pain already, and for people who are transitioning to barefoot walking. They should be performed for about one minute each, on both feet, 1-2x per day (so about 10-20mins). Whether you have foot pain, want to try walking barefoot, or just want to treat yourself - I encourage you to try them, because they feel so good! Or, if you have a loving partner or a really, REALLY good friend… ask for swapsies!  These days, there are many barefoot (“minimalist”) shoes available. These are designed to mimick and maintain the natural shape of the foot, and keep you as closely connected to the earth as possible, to allow the biomechanical benefits of barefoot walking, whilst also offering your feet protection. They are becoming more widely available in many different styles to suit every occasion and purpose, and have come a long way from the classic “toe shoes”. However beware, not all minimalist shoes are made equal, and some may share design flaws similar to that of conventional shoes (see my previous blog post!), so I highly recommend speaking to your local podiatrist or other foot-savvy health practitioner before deciding on a pair. 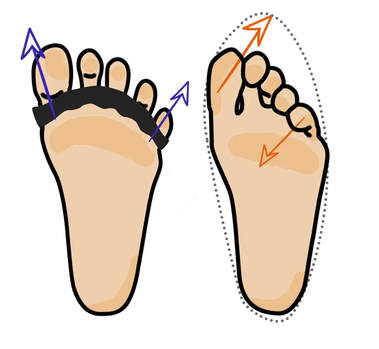 One more useful appliance which complements the barefoot movement are toe spacers. These are basically designed to prevent, and slowly reverse, any changes to the forefoot sustained by conventional footwear… and more specifically those sexy but pesky narrow toe boxes. They can be helpful in alleviating a wide variety of foot pain from bunions, hammertoes, other types of crooked toes, hallux valgus, ingrown toenails, sesamoiditis, neuromas and capsulitis, as well as having encouraging the change responsible for many of the benefits of barefoot walking. Similarly to barefoot walking, your foot needs to adjust to using toe spacers. One can start by wearing the spacers for shorter amounts of time and progress as comfortable. Start with 30-60 mins for 2-4 weeks. You can wear them in a variety of settings, including: In bed while sleeping, lounging around the house, during yoga and other barefoot workouts, at the beach, outdoors as part of a grounding practice. It is also important to note that toe spacers are not compatible with all shoes and should NOT be worn in conjunction with orthotics or arch supports. Although orthotics and toe spacers share similar goals (offering support to areas of the foot and stabilising foot arches), orthotics do this in a passive process which opposes the active process in which toe spacers work. Please speak with a foot specialist before trying toe spacers to find out if they can be helpful for you. 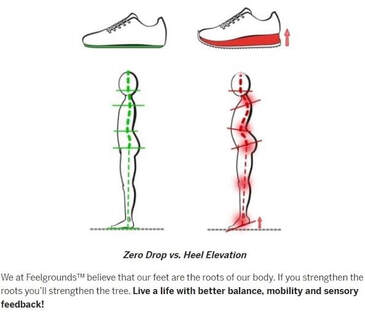 By Angus Nicol Remember that the shape of our shoes, alongside all the added cushion and support, alter our normal walking pattern. Well guess what? Walking barefoot can help return them back to normal (in time). When you walk barefoot, more of your foot makes direct contact with the ground. This means that more proprioceptors (the nerve endings responsible for knowing a body parts “position in space”) are stimulated - leading to improvements in body awareness and balance, and reducing pain. It also means that you’ll be more weary and have more control when your foot strikes the ground. The freedom and lack of rigidity associated with barefoot walking means that all the joints are free to move through their full range of motion, and over time the muscles in your legs and your feet will get stronger. Consequently, you will gain a more stable arch and improved foot mechanics; and have a flow on effect of potentially reducing the chance of injury and decreasing pain further up the chain in the knees, hips and low back. All of these changes lead to restoration of a normal walking (gait) cycle, happy soles… and some research suggests happy souls too (read on!). I bet that sparked your interest, how could walking barefoot make my soul happy? That sounds a bit far fetched, and yes… I might be exaggerating a bit, but it sounds good, right? And it’s pretty accurate! Outside of the biomechanical advantages of barefoot walking, the process of “grounding” or “earthing” is another understated advantage of stomping around on Mother Earth - the greatest healer. We humans, like all other living creatures, are bioelectric beings. I won’t dive too deep on the sciencey stuff… all you need to know is that the human body carries a slightly positive charge, and the earth carries a slightly negative charge with an abundance of free electrons (who doesn’t like free stuff?!). Direct contact with the earth allows transference of these electrons and expulsion of excess electricity in the body. There is currently limited research in this area, however the available research isshowing some incredible findings! 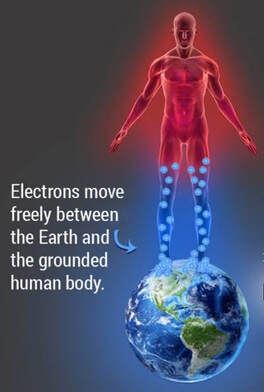 Firstly, the transference of electrons from the earth to the body may help to neutralise free radicals (unpaired electrons) in the body, similarly to antioxidants, and relieve oxidative stress, thereby supporting healthy immune function. Grounding has been reported to increase energy and decrease fatigue, decrease cortisol (a slow release, long term stress hormone), decrease inflammation, increase circulation, decrease blood pressure, improve sleep and mood, lessen depression/anxiety, and lead to faster injury and wound healing times. Although further research is needed, emerging evidence is promising and risk free! In addition to barefoot walking, other ways to practice grounding are by laying on the ground (think star or cloud gazing, picnics, sun bathing etc), immersing yourself in natural bodies of water (beaches, lakes, rivers etc). Grounding indoors is a little more challenging, however there are now products available such as grounding mats, blankets, socks and patches that give you more access to these benefits.  Now, sticking to a more energetic approach, barefoot walking may also provide benefits working within a Traditional Chinese Medicine (TCM) paradigm. Have you ever heard of, or experienced, foot reflexology? It works on the premise that particular areas of the foot correlate with specific areas of the body. When pressure is applied to these areas, they are stimulated and vital energy (or “Qi”) flows to the corresponding area of the body, helping return the body back to balance and allowing the body to self heal. The scientific evidence supporting foot reflexology is weak and not significant, however it is reported to share similar benefits to those of grounding. When you stand barefoot (especially on uneven surfaces) for an extended period you will apply pressure to different parts of the foot, thus initiating the Qi cascade to the corresponding area of the body. Whether it be biomechanical, through grounding/earthing, or via TCM foot reflexology principles, there is no doubt that barefoot walking has a plethora of far reaching benefits throughout many areas and systems of the body. Please see Part III of this blog to see how you can safely start your barefoot journey!  By Angus Nicol What are your favourite pair of shoes? Are they your reliable, extra cushioned and supportive runners, your convenient and trusty thongs (or whatever you want to call them… pluggers, sandals, jandals) or styley Birkenstocks; your super fly leather boots or bootylicious high heels; or the cosiness of a good pair of fur-lined slippers/uggs? Or… do you prefer feeling the ground beneath your feet and the freedom which comes with walking barefoot? Your feet are so important. They are your first and main point of contact with the earth, and they carry the weight of the rest of the body… so having foot problems can contribute to compensatory problems throughout the rest of the body! Therefore, it is important to take care of them. I’m not here to tell you to throw all of your shoes away… they all serve their purpose. However, in this blog I would love to illuminate the features and limitations of modern conventional footwear, and conversely, and in Part II highlight the benefits of barefoot walking/using minimalist footwear, and also discuss how to ease into the transition. 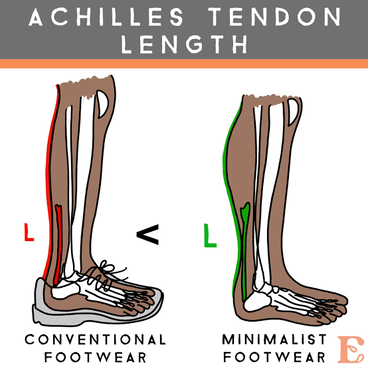 Before we go into the benefits of walking barefoot, I feel it’s important to understand shoes. I want to show you the different parts of a shoe and what their function is, and then tell you the negative effect they may be having on your feet. To try and keep it flowy, I’ll start at the back and work my way forward, and then out. The heel of many conventional shoes are thick, causing them to be more elevated than the front. The most extreme example of this is high heels, however it is present in most forms of footwear, including mens boots and most runners. Elevated heels were designed to provide cushion & support, thus providing more comfort. They also act as a shock absorber, so less force is transmitted into the heel, ankle and up through the rest of the body. Sounds ideal, right? Maybe… but there are some negative consequences which potentially outweigh these benefits. This includes shortening (and consequently “tightening”) of calf muscles. If muscles are shortened, they are unable to contract fully and strongly, so this also decreases the efficiency and strength of these muscles. They also reduce the amount of natural arch support, particularly in the main arch of the foot (the medial longitudinal arch aka MLL), which leads to the foot turning in too much (“overpronation”). Overpronation is made worse in shoes with a narrow toe box (keep reading, you’ll learn about this soon). 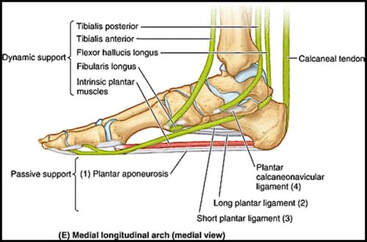 The middle part of the shoe, where your arch sits, is called the midsole. The midsole of many shoes, particularly runners, will include an inner sole (the spongy layer of foam in the bottom of the shoe) that has arch support. This arch support may be necessary due to the heel elevation and collapse of the MLL, or helpful for people with “flat feet”. However, these act as a band-aid solution to the underlying issues in the foot leading to collapsed arches. Furthermore, over time your body will adapt and may become reliant on this arch support, and the small muscles which should provide stability and maintain this arch can become lazy and weak, causing excerbation of the issue. 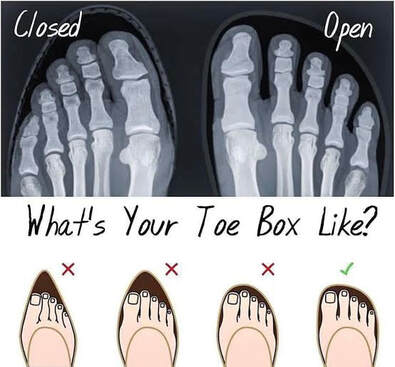 The front part of the shoe, the part that houses your toes, is aptly named the toe box. It may be sleek and stylish to have a narrow toe box that ends in a tapered point. However, this is like your forefoot having a giant squishy hug from a grizzly bear, causing compression of the bones and joints in the toes and the foot. Narrow toe boxes are a leading cause of foot injuries/conditions including bunions, hammertoes, plantar fasciosis, neuromas and ingrown toenails… just to name a few. However, the negative effects can be seen further up the kinetic chain too, and may contribute to knee osteoarthritis, shin splints and runners knee. The very end of the toe box, where the toe is pointed upwards, is known as the toe spring. It is designed to decrease rigidity of the shoe, allowing us to flow easily from heel-to-toe for a nice smooth walking pattern. However, the elevation at the front means our toes have less contact with the ground, so when shift our weight towards the toe box, most of the force is being absorbed by the metatarsals (the bones that connect our toes to the rest of our foot), which can cause or contribute to many of the conditions mentioned above. 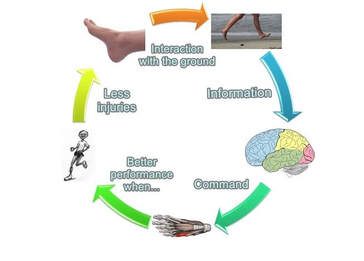 The outermost layer of the bottom (sole) of the foot is the outsole, this is the part that directly contacts the ground. These are often designed with materials that provide cushion and rigidity. However, the more cushion there is in a shoe, and the more rigid it is, the less contact and “feel” your foot has with the surface underneath. Our feet are filled with tiny nerve receptors called proprioceptors, which provide feedback to our brain about joints (and our body as a whole) “position in space”, and contributes largely to our sense of balance. Our brain receives information from proprioceptors and responds by sending messages to our muscles to contract, allowing movement in all directions, and adaptation of our feet to the surface below. The rigidity of an outsole only allows the foot to flex and extend, and less contact area between the foot and the ground means less proprioceptors are stimulated, which means that the brain receives less sensory information and less movement messages relayed back down the chain. Over time this can lead to weakening and atrophy (shrinkage) of the muscles that stabilise the arches of the foot. Phew… that was a lot to take in. Are you still with me? The good news is, that’s the hard part done. Next, I want to tell you about the benefits of walking barefoot… which to an extent, is just the reverse of the limitations of wearing footwear (plus a few extra little goodies!). Please see Part 2 of this Blog Post for the benefits of barefoot walking, how to start your barefoot journey, and some other helpful tips and hints.  By Kirby Edwards Why would a teenager need to see an osteopath? Osteopathy for teenagers looks at structure, function and movement in relation to everything else. We look at those complex relationships through the body, including the bones of the head, pelvis, limbs and torso. As we transition through puberty, it can be a challenging time. A lot of changing hormones (and heightened emotions), challenging environments, growth spurts and often compounding injuries of falls and traumas from adolescence.Before we put our hands on, we will talk to the teen and the parents about the birth and pregnancy, medical history including any allergies, falls, broken bones and family history, sleep patterns to gain as much information as we can. We might even ask about your bowel movements or menstruation (horrified gasp!)  How do you treat a teenager? As osteopaths, we have a variety of tools in our toolkit for treatments and often use a combination. We may use cranial osteopathy or biodynamics, which is a gentler approach that helps the body to find better balance optimise movement. We may use soft tissue techniques such as massage, muscle tension release or stretching. Other techniques we may perform include joint mobilisation, muscle energy techniques or myofascial techniques. Education and advice to manage your condition between appointments is often provided, as well as some take home exercises. What can an osteopath do for teenager? Osteopaths can support teenagers with a variety of issues:
 What can I expect post treatment? As with any treatment for anyone, there is an adjustment period to the new balanced normal. Each person can react differently. It can take between 1-3 days to settle down, although for some may settle down straight away. Feel free to give us a call if you have any questions. We may also send you off with a referral to a GP or another specialist if the issue is out of our scope. 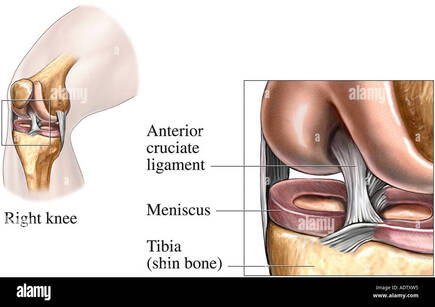 By Liam Neyland What is the ACL The anterior cruciate ligament (ACL) is a dense band-like connective tissue designed to attach the bottom of the femur to the top of the tibia. The ACL is one of the major structural aspects of the knee, it’s main function to resist rotational loads and anterior tibial translation (stop the shin bone falling forward). Despite being only one of the four major ligamentous structures of the knee, injury to the ACL is one of the most common knee injuries in Australian sport. It is so common in Australia that we lead the world in reported ACL injuries, with an increase of 70% in the last 15 years according to studies. Between 2000 and 2015 a reported 200 000 ACL reconstruction surgeries were performed which on average has an annual cost of 142 million a year to the medical system.  How does an injury occur? Despite the fact that the most common demographic who suffer from ACL injuries are young athletes in contact sports , the majority of injuries are non contact in nature. Approximately 70% of all ACL injuries are non contact with most occurring from a plant and pivot motion. The ACL is put under further stress if these movements are performed during rapid deceleration into acceleration. Females are 3 times more likely to have an ACL injury for a number of reasons, including ligament laxity. The severity of an ACL injury is classified into 3 separate grades; grade 1 is a stretched ligament without any tears occurring, grade 2 is a partial tear and a grade 3 is a full tear.  How is it diagnosed? Most ACL injuries can be diagnosed from a comprehensive history taking and physical examination, which can be performed either by a GP or by a manual therapist like an Osteopath. The examination would include a few orthopaedic tests that are designed to stress the ACL to determine how much laxity is present or if the ACL is still intact. A GP or manual therapist may refer for extra tests such as an MRI, x-ray or ultrasound for confirmation of the diagnosis or if they suspect other structures of the knee may be damaged as well which is common with most ACL injuries.  How can an Osteopath help? The severity of the ACL injury will be the main factor in determining what treatment approach may take place. For low level injuries the use of manual techniques such as articulation, contraction/relaxation and soft tissue work may be used to reduce inflammation and decrease overall pain. For a higher level injury, including full ruptures, the treatment approach may differ as an ACL reconstruction may be required. If surgery is not warranted by a specialist or not preferred by the patient then treatment would involve the implementation of an exercise and rehabilitation program which may focus on prevention of further injury. These programs may be designed to strengthen muscles that may have been a driving force for the original injury or to correct poor mechanical movement and alignment of the knee as well as other major joints of the body. If surgery has already been performed a rehabilitation program can still be used for treatment with the main goal focusing on return to sport or work. If you are suffering from an ACL injury, the Osteopaths at HMC Osteopaths are happy to help using their knowledge and experience with treating several different sporting injuries. References Increasing rates of anterior cruciate ligament reconstruction in young Australians, 2000-2015 - PubMed (nih.gov) ACL injury - Diagnosis and treatment - Mayo Clinic The biomechanics of ACL injury: progresses toward prophylactic strategies - PubMed (nih.gov) Anterior Cruciate Ligament (ACL) Injury - Physiopedia (physio-pedia.com)  By Kirby Edwards You may have heard us speak of inflammation. Inflammation is when your body activates the immune system. It sends out inflammatory cells which are helpful in fighting against things that harm you. These can include bacteria, viruses, toxins (such as alcohol), fungi or damaged tissue from trauma. When your body sends out inflammatory cells when you are not sick or injured, you may have chronic inflammation. I like to think about the immune system in a very simplistic way, a fire fighter. Sometimes the body has lots of little fires (inflammation) and as a result of trying to fight lots of little fires, it cannot put any of them out entirely. Its overworked and spread too thin. We may need to make some modifications to give it a fighting chance.  Alcohol is just one of the things that can contribute to excessive inflammation. The body is incredibly resilient (I mean think about what we put it through and put into it daily and it still functions – amazing!) So, if you are constantly struggling with inflammation, perhaps removing/decreasing alcohol is the one thing that we have not noticed or removed. Removing the booze for a while or cutting back has some significant health benefits: it improves sleep, can result in weight loss, improve energy levels, lessen anxiety, better hydration (and skin often improves here too), save money, improve cognition, stomach may feel better/decrease nausea and reflux, your liver will be healthier. Some of us have never taken any time off the booze, it has just always been there in the background, either as 1-2 per day or just on the weekend. 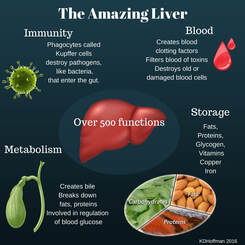 Your liver has so many amazing functions, some of which you may know, including processing alcohol and other poisons. What you may not know is that it also helps the body to remove contaminants, regulate hormones, helps filter the blood and has an impact on blood pressure, helps with digestion by producing proteins, enzymes and bile, stores minerals and vitamins and assists the immune system, just to name a few of over 500 functions. So, by removing alcohol, it gives your liver one less job (minimum) to do and allows it to get back to all its other jobs, including assisting the body to decrease inflammation, not to mention saving money! 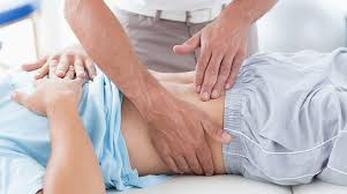 So, what’s the connection to Osteopathy and Alcohol? Well, as you know, Osteopathy looks at the body as a whole and what you put into your body is something that can really affect you. Aside from taking a break from the booze, we do suggest that you do not drink for 24-48 hours after a treatment. The treatment keeps tinkering away for following 24-48 hours after we see you and at this time, we encourage you to nourish your body, including drink lots of water, eat well and get some good sleep. For those of us considering taking a break from the booze. Here are some resources: A few Sobriety books or “Quit lit” :
A few websites/instagram to check out:
A list of places you can go and join ‘challenges’ or experiment:
A list of podcasts:
There is also:
So there is some resources, with July right around the corner, why not give Dry July a try? 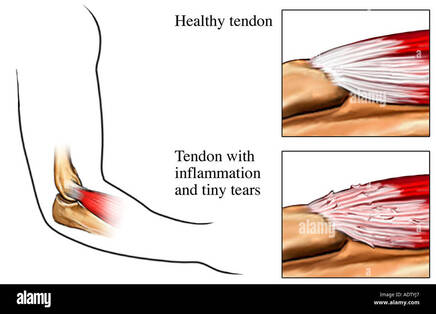 By Liam Neyland So, what is it? Lateral epicondylitis, or more commonly known as 'tennis elbow', is a condition where the tendons of the elbow become inflamed resulting in pain occurring during certain motions or during restful periods. Despite the name ‘tennis elbow’ this condition is quite common among the general population and is not exclusive to athletes. The pain that people feel when suffering from tennis elbow occurs most commonly at the bony bump located on the outside of your elbow where the tendons of the extensor muscles attach. This pain can be quite erratic with some presentations only at the elbow, or at both the elbow and other areas such as the forearm and wrist.  What are the symptoms? The most common symptom that presents when suffering tennis elbow is pain, along with a decreased grip strength either due to pain or generalised weakness. The pain experienced from tennis elbow can range from either a burning sensation, sharp, stabbing and or a dull ache just to name a few examples. A major indicator of tennis elbow is experiencing pain when performing tasks such as holding a cup of coffee, turning a door knob and or shaking someone's hand.  What causes it? The most common cause of tennis elbow is simply the overuse of the extensor muscles. When performing repetitive actions such as typing, using hammers or playing a musical instrument these motions can result in the tendons of the extensor muscles becoming inflamed. This normally is not an issue as the body will naturally repair any damage done to the tendon. However, if the tendon is not allowed ample time to heal this inflammation can progress to microscopic tearing. This in turn makes the pain experienced more pronounced and or generalised along the forearm, and increases the time needed to properly heal. 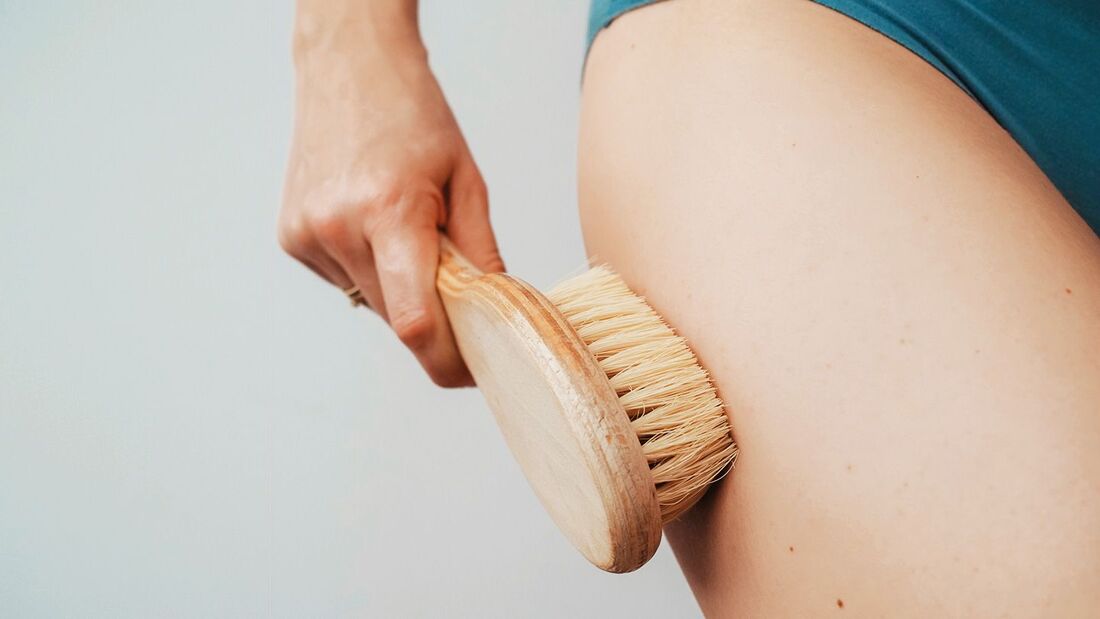 How is it diagnosed? The most time efficient and simple way to determine if you may be suffering from tennis elbow is to have a physical exam performed. These exams can be performed by Doctors and most if not all Manual Therapists such as Osteopaths. After these examinations it is not uncommon for a Doctor or the Manual therapist to suggest some form of x-ray or MRI. These tests are mostly used to help identify any factors that should be considered before commencing treatment such as calcification of the tendon or to simply confirm the diagnosis.  How can an Osteopath help? An Osteopath can implement a wide range of treatment options that are dependent on the stage of the condition as well as how complicated it is. For early stages advice and lifestyle changes are normally implemented along with hands on treatment such as soft tissue or myofascial release to name a few. For more advanced stages of the condition the previous treatments can still be used but would be implemented in conjunction with rehabilitation programs that may or may not involve the use of other treatment methods such as dry needling. If you have been suffering from elbow pain and this sounds familiar to you, the Osteopaths at HMC Osteopathy are happy to help you and are equipped with knowledge and experience to treat any and all complaints. References: Lateral Epicondylitis - Physiopedia (physio-pedia.com) , Tennis elbow - PMC (nih.gov), Tennis elbow | healthdirect  By Kirby Edwards Why would a baby need to see an osteopath? Osteopathy for babies is a gentle non-invasive hands-on approach to treatment. Babies (and Mums) may retain tension in their tissues (muscles, fascia, vessels, bones) from the birth and other experiences. This may be quite uncomfortable. Osteopathy looks at structure, function and movement of the tissues. By looking at those complex relationships through the body, including the bones of the head, pelvis, limbs and torso, Osteopaths can aim to optimise the body’s own self-healing and self-regulating mechanisms. Before we begin hands-on therapy, we will talk to the parents about the pregnancy, birth, medical history of the baby and family, feeding and digestion, sleep patterns and movements of the baby to gain as much information as we can as well as answer any questions you have. Osteopaths will assess how the body is generally moving, respiration, cranial bones of the skull and possibly check inside the baby’s mouth to check out the tongue. What can an osteopath do for babies? Osteopaths with a special interest in newborns and paediatrics can support and assist newborns or infants in a variety of issues:
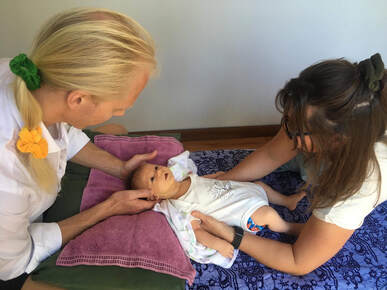 How do you treat a baby? As babies are still very flexible and mostly cartilaginous bones, we do not perform any type of sharp manipulation or firm treatment. Our approach to babies is much gentler, often using cranial osteopathy or working with the fluid dynamics or fascia of the body to release any tissues that are under tension and restore optimal balance to the baby. We may place our hands on their rib cage, pelvis or skull. We can also work with tensions around the mouth and jaw to optimise feeding and digestion for the baby. We work closely with lactation consultants and other professionals should there be any other issues, such as a tongue tie release being required. The long-term implications of tongue ties can influence the jaw and palate development and position altering how the baby’s airways are forming, thus leading to altered or suboptimal posture breathing mechanics. It can also lead to too much air in the baby’s tummy and discomfort (as a result, excessive screaming). 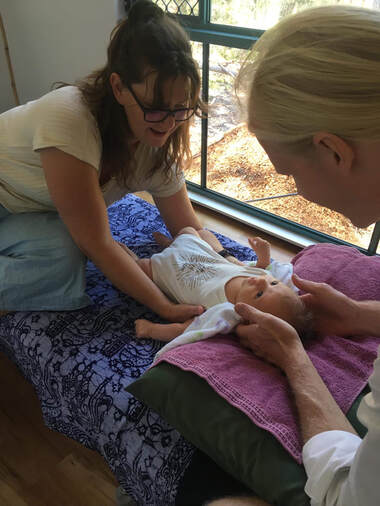 What is cranial osteopathy? This is a gentle hands-on treatment that helps the body to find better balance and optimise movement. Osteopaths are trained to develop their palpation skills. With Osteopathy in the Cranial Field (OCF) we are trained to feel subtle motion in the whole body. This is called the Primary Respiratory Mechanism (PRM). Although the name is ‘cranial,’ this mechanism can be felt and worked on from anywhere in the body. One of the principles of Osteopathy is that it is all connected. Osteopaths see connections between different parts of the body and by working with this principle aim to optimise the body’s function. OCF is a subtle refined approach that can affect all systems of the body aiming to restore balance and health. Cranial Osteopathy can be of benefit for everyone, but due to its gentle effective approach is ideal for babies and children. What can I expect post treatment? As with any treatment for anyone, there is an adjustment period to the new balanced normal. Each baby (and person) can react differently, but often they are very sleepy, hungry or maybe a little agitated. It can take between 1-3 days to settle down, although some may settle down straight away. Feel free to give us a call if you have any questions. We may also send you off with a referral to a GP, midwife, or lactation consultant, if the issue is out of our scope. |
HMC TEAMIf you find something of interest that might suit this space, or would like information on a specific topic, let us know at [email protected]
Archives
December 2023
Categories |




 RSS Feed
RSS Feed
